Bowel Function & Pelvic Health: The Underappreciated Link

Anorectal or bowel dysfunction is common, yet is under-reported, under-diagnosed and under-treated. Nearly 2% of Australian adults experience faecal incontinence and 4% experience both urinary and faecal incontinence1. A staggering 40% of the world’s population are impacted by Disorders of Gut-Brain Interaction (DGBI) eg Irritable Bowel Syndrome (IBS)2.
Other pelvic health conditions such as urinary incontinence, pelvic organ prolapse and pelvic pain often co-exist with bowel disorders. Therefore, any pelvic health condition should consider bowel function during assessment and management.
The Wide Spectrum of Anorectal Presentations
- Faecal / flatal incontinence
- Involuntary loss of faeces (solid or liquid), flatus, passive faecal incontinence (soiling without sensation or warning or difficulty wiping clean)3
- Faecal urgency
- Sudden, compelling desire to defaecate that is difficult to defer3
- Feeling of incomplete evacuation
- Complaint that the rectum does not feel empty after defaecation3
- Straining to defaecate
- o The need to make an intensive effort (by abdominal straining or valsalva) to either initiate, maintain or improve defaecation3
- Constipation:
- Complaint that bowel movements are infrequent and/or incomplete and/or there is a need for frequent straining or manual assistance to defecate, based on Rome IV diagnostic criteria of4:
- Two or more of the following:
- Straining more than 25% of defaecations
- Lumpy or hard stools
- Sensation of incomplete evacuation more than 25% of the time
- Manual manoeuvres to assist with emptying more than 25% of the time
- Less than 3 spontaneous bowel movements per week
- Two or more of the following:
- Loose stools rarely present without laxatives
- Insufficient criteria for IBS
- Complaint that bowel movements are infrequent and/or incomplete and/or there is a need for frequent straining or manual assistance to defecate, based on Rome IV diagnostic criteria of4:
- Rectal Prolapse
- Protrusion of the rectum beyond the anus3
- Persistent Anorectal Pain4,5
- Levator Ani Syndrome
- Persistent or recurrent rectal pain, lasting more than 30 minutes, with tenderness with traction on puborectalis muscle
- Proctalgia Fugax
- Recurrent episodes of rectal pain unrelated to defaecation that lasts from seconds to minutes (maximum 30 mins), with no pain between episodes
- Levator Ani Syndrome
- Irritable Bowel Syndrome (IBS)4
- Recurrent abdominal pain on average at least 1 day/week in the last 3 months, associated with two or more of the following criteria:
- Related to defecation
- Associated with a change in frequency of stool
- Associated with a change in form (appearance) of stool
- There are different subtypes of IBS characterised by predominant bowel habits (constipation, diarrhoea, mixed or unclassified)
- Recurrent abdominal pain on average at least 1 day/week in the last 3 months, associated with two or more of the following criteria:
Anorectal Dysfunction Doesn’t Always Present As The Main Problem
The Relationship Between Pelvic Floor Muscle (PFM) Dysfunction & Anorectal Conditions
- Increased tone of the PFM which may result in poor relaxation during defaecation and contribute to incomplete emptying
- Weakness, poor support and increased descent of the PFM and connective tissue, impacting the mechanics of defaecation
- Poor coordination of the PFM, where the muscle contracts when it should be relaxing (defaecation dyssynergia) or vice versa
- In some cases, PFM function is completely normal and the constipation is due to other factors
- A digital rectal examination (DRE) to determine resting muscle tone, ability of the EAS and levator ani to contract and relax (at the right time), endurance and coordination
- Observation of the perineum in a sitting position on a commode to understand structural support and defaecation dynamics
- Transperineal ultrasound to visualise the anorectal angle, levator plate, PFM contraction, relaxation and coordination during simulated defaecation
- Abdominal palpation to assess the tone, activity and co-ordination of the abdominal muscles during breathing and simulated defaecation
- Breathing pattern observation and assessment
Chicken Or The Egg: Psychosocial Implications
- Fear of leaving the house if they haven’t emptied their bowel in the morning
- Avoiding eating or drinking food if they are planning on going out for fear of having an accident or an episode of urgency
- Needing to know where the closest toilet is at all times
- Feeling that their day is ruined if they haven’t emptied their bowel in the morning
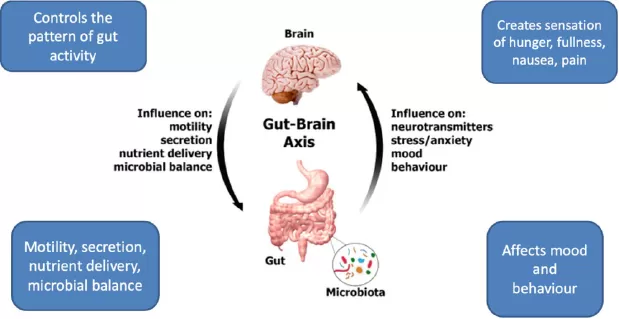
The Integral Relationship Between the Brain and the Gut
- from the brain to the gut carrying messages that control the pattern of gut activity
- from the gut to the brain creating sensations of hunger, fullness, nausea, pain, all of which can affect mood and behaviour
Trauma and Anorectal Dysfunction
- Prior to any assessment:
- Screen for trauma
- communicate and obtain initial informed consent
- Answer questions and validate concerns
- Cultivate a trauma informed environment
- During any assessment
- Obtain ongoing consent
- Monitor for signs of distress or dissociation
- After assessment
- Debrief with the patient
- Provide a written summary
- Refer for psychological support if needed
Anorectal Dysfunction Requires A Biopsychosocial Approach
- Education
- Understanding normal bowel function can reduce fear and anxiety associated with symptoms
- Awareness of the gut-brain axis, the nervous system, pain system and musculoskeletal system and how they interact with emotional health and gut function
- Breathwork
- Diaphragmatic breathing can regulate the coordination of the diaphragm and PFM to descend and relax at the right time during defaecation
- Breathwork is an effective strategy to move out of a sympathetic state of flight or fight and into a parasympathetic state of rest and digest
- Defaecation dynamics
- Teaching correct defaecation dynamics is more than instructing someone to elevate their feet and bulge their belly when they sit on the toilet
- Technique must be assessed and the retraining individualised to ensure generation of enough rectal pressure without compromising pelvic floor support
- Establishing an effective bowel routine
- Many people don’t appreciate the importance of a routine that takes advantage of the HAPC – high amplitude propagating contractions of the smooth muscle of the bowel that occur upon waking and after meals
- PFM training (PFMT)
- The goal of PFMT may be to improve awareness, strength, relaxation, coordination or endurance
- PFMT will always be linked to functional requirements
- Application of adjunctive therapy ie Electrical Stimulation
- Biofeedback for PFMT can be provided via:
- Verbal instruction and feedback
- Palpation via DRE/abdomen
- Visual feedback via transperineal ultrasound
- Per rectal EMG biofeedback
- Rectal Balloon Therapy
- Rectal Balloon Assessment and Therapy
- To assess rectal sensation, compliance and defaection dynamics
- For sensory and/or defaecation retraining
- Abdominal massage has been shown to increase the frequency of defecation, improve defaecation dysfunction, stool consistency and quality of life11
- Urge Suppression Strategies
- To assist in calming the urgency sensation and break the fear-urge cycle
- Stool Manipulation
- Working in conjunction with a GP, dietician or medical specialist, we explore strategies to optimise stool consistency, within the scope of our clinical expertise
- Strategies to calm a sensitised nervous system
- Mindfulness, whole body movement practices, general exercise, sleep hygiene, stress management and more
Regardless Of Your Discipline, We All Should Care About Bowels